Cortisol is the primary stress hormone that fine-tunes our response to the stress of everyday living. However, it serves an important role in other important functions.
Cortisol is a steroid hormone, one of the glucocorticoids, made in the cortex of the adrenal glands and then released into the blood, which transports it all around the body. Almost every cell contains receptors for cortisol and so cortisol can have lots of different actions depending on which sort of cells it is acting upon. These effects include controlling the body’s blood sugar levels and thus regulating metabolism, acting as an anti-inflammatory, influencing memory formation, controlling salt and water balance, influencing blood pressure, and helping the development of the fetus. In many species, cortisol is also responsible for triggering the processes involved in giving birth.
A similar version of this hormone, known as corticosterone, is produced by rodents, birds, and reptiles.
Daily Cortisol Curves
A commonly used tool for assessing adrenal hormones is a diurnal cortisol curve. This curve is derived from taking four daily saliva collections – typically done upon waking, before lunch, before dinner, and before bed – and charting them on a 24-hour graph.
The resulting curve – also called a four-point cortisol curve or circadian cortisol pattern – reveals cortisol levels throughout the day and allows health care providers to pinpoint issues with adrenal gland function.
Cortisol Awakening Response (CAR)
The Cortisol Awakening Response – also called CAR – reveals more detailed clues that help in assessing adrenal hormone/HPA Axis dysfunction. This testing is often useful for cases of PTSD, major depression, chronic fatigue syndrome, and other severe stress conditions.
During a normal cortisol awakening response, adrenal hormone levels should increase 50% in the first 30 minutes after waking for the day and then begin to progressively drop through the afternoon and evening. To capture this response, three – rather than one – morning saliva collections are needed to properly chart the diurnal cortisol curve.
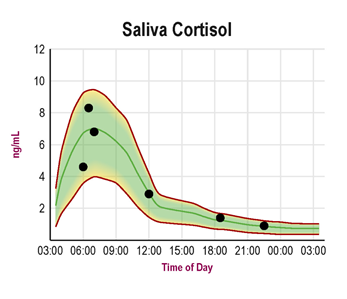
This pattern shows a normal rise in cortisol production within 30 minutes of waking for the day. Cortisol levels then drop throughout the day, reaching their lowest point at bedtime.
Daily Cortisol Patterns with Adrenal HPA Axis Dysfunction
Cortisol production is normally at its highest 30 minutes after waking and declines steadily during the day, reaching its lowest point at bedtime. Those with adrenal gland dysfunction generally have irregularities in their diurnal cortisol curves. Some common examples are shown below.
Overall higher than normal cortisol production throughout the day can result from prolonged stress demands. General symptoms include feeling “tired but wired,” food cravings, insomnia, and anxiety.

The pattern for chronic fatigue shows elevated morning cortisol with levels dropping off rapidly during the day. General symptoms include mid-day energy drop, drowsiness, and poor exercise recovery.

The burnout pattern, also commonly called “adrenal fatigue” is really a reflection of low overall cortisol during the day. General symptoms include day-long fatigue, irritability, food cravings, insomnia, and exhaustion.

One Lab Me health check that measures cortisol 4 times throughout the day is the sleep disturbance test.
What Do Cortisol Fluctuations Mean?
Cortisol is the main glucocorticoid hormone that is secreted by the cortex of the adrenal gland and is the most important one.
Synthesis and secretion of cortisol are controlled by adenohypophysis hormone, adrenocorticotropic hormone, ACTH, while the synthesis and secretion of ACTH are controlled by hypothalamus hormone, corticotropin-releasing hormone, CRH.
- Cortisol has its highest levels in the morning and lowest in the evening.
- Both physical and psychological conditions affect the cortisol rhythm.
- ACTH and cortisol can be secreted independently of circadian rhythm as a reaction to physical and psychological stress.
- Higher concentration of cortisol and lack of daily rhythm can be identified as Cushing’s Disease.
- As well as in patients with adrenal tumors, low cortisol concentration can be found at primary insufiation of adrenal core gland (Addison’s disease) and lack of ACTH.
The results of our measurements have shown the lower value of cortisol concentration in the afternoon hours in comparison to the measurements in the morning in samples of saliva, as well as in samples of saliva.
Is Cortisol Reliable By Saliva Measurements
Besides the measurements of blood and urine, the measure of cortisol concentration in saliva has recently become an important choice in many analyses.
Taking the samples of saliva has many practical advantages because cortisol in saliva can be measured under many clinical and practical conditions. It is believed that cortisol enters the saliva by passive diffusion or in other ways independent of active mechanism transports, the concentration of cortisol in saliva remains unchanged depending on the amount of saliva that is formed.
According to the concept of free hormone only unbound cortisol comes to the target tissue and forms the reaction of glucocorticoid effects. Recently, many scientists and endocrinologists have examined new methods and applications of cortisol concentration measurement of cortisol in order to have additional proof of the importance of cortisol measurements in saliva.
This will encourage wider cortisol measurements in basic and clinical psycho-endocrinological examinations. Despite the fact that many researchers have shown that there is a correlation between the concentration of cortisol in saliva and the concentration of cortisol in plasma and serum, certain doubts still exist. The results that support this theory are shown in the body fluids of healthy persons.
High correlations between saliva and serum cortisol are noticed in newborns, children, and adolescents, elders, as well as psychiatric patients.
Most studies show that the amount of saliva cortisol is connected with the amount of cortisol in the blood, but the absolute cortisol concentration that is found in saliva is much lower than the cortisol concentration in blood in all studies.
Results of our measurement have shown a lower cortisol concentration in samples of saliva in comparison to concentrations of cortisol in samples of serum, as well as in samples that were taken before noon and afternoon hours.
It can be concluded that measurements of saliva cortisol in early morning hours could completely replace measurements of cortisol in serum and plasma.
Diurnal Cortisol Curve Assessment
Thirty minutes after awakening from a good night's sleep, cortisol levels are at the highest they'll be all day. Following the morning peak, cortisol levels then fall to less than half that peak level by noon.
They continue to drop to very low levels at night where they stay low during the sleep hours. Some individuals have a sharp rise to reach morning levels, others a more gradual incline.
Looking at cortisol levels graphed during the day, any abnormal elevation, or depression of levels, or a loss of the expected curve with its characteristic morning peak and swooping decline towards evening may suggest HPA axis dysfunction – which is what we're most interested in assessing when we're looking at a diurnal cortisol curve (i.e. a 4-point cortisol test).
Looking at the diurnal curve of saliva cortisol levels plotted against time of day can give us some useful information about the body's response to chronic stress and the ultimate downregulation of pituitary ACTH, but an altered diurnal cortisol curve could also be due to more acute stressors.
Some examples of things that affect the 24-hour cortisol pattern include:
- Dysglycemia or even fasting a little too long between meals
- Sleep
- Exercise
- Pain
- A recent cortisone injection or regular topical, inhaled or oral steroid use
We expect onslaughts to the HPA axis to yield predictable results – the highs and lows following each challenge should tell us the HPA axis is functioning properly. In the face of severe chronic stress, we expect to see high cortisol levels throughout the day.
When we see normal or low cortisol levels instead, we suspect HPA axis dysfunction. We do our best to put together an individual's symptoms with what the 4-point cortisol curve is telling us to help guide treatment decisions. But sometimes it just doesn't add up and we need more information.
What if you could add several more saliva collections to see how cortisol is changing in the first hour or so upon awakening?
A Second Measure of HPA Axis Tuning
Cortisol Awakening Response (CAR) gives us even more clues to pin down the reason for a hyperactive or hypoactive HPA axis.
How can we assess the response capacity of the HPA axis?
We have a built-in mechanism governed by the hippocampus and the light-sensitive suprachiasmatic nucleus of the hypothalamus wherein cortisol levels show a temporary boost between the moment of waking and 30 or so minutes after rising, returning to the initial waking level at 60 minutes after waking.
This transient rise in cortisol levels is unique to the stimulus of morning waking. It doesn't happen when we are woken from sleep in the middle of the night or after we take an afternoon nap. It happens in the first hour or so after waking up, and it's called the Cortisol Awakening Response (CAR). The magnitude of the CAR gives us some idea of the HPA axis's ability to activate and respond to the magnitude of all the stressors (normal physiological stress, self-perceived emotional stress, physical stress, etc.) that face us as we awaken and begin the day.
CAR gives us even more clues to pin down the reason for a hyperactive or hypoactive HPA axis.
So, what is a NORMAL CAR response?
On awakening, cortisol should increase about 50% in the first 30 minutes then begin to progressively drop the remainder of the day.
Three, rather than one, early morning collections are what is needed to accurately assess the CAR; one immediately on waking, one 30 minutes later, and another at 1 hour.
The other three collections are done as usual – before lunch, dinner, and bedtime.
Clinical Use of CAR
Decreased CAR has been associated with the following conditions:
- PTSD
- Chronic Pain
- Systemic hypertension
- High CIMT (carotid intima media thickness) in women
- Functional GI diseases
- Postpartum depression
- Chronic Fatigue Syndrome
- Major depression
- Insomnia (but not isolated night waking)
- Autoimmune diseases
- Atopic and allergic conditions
- Low frequency noise exposure
- Low socioeconomic status
- Perceived high stress
- Cushing's Disease
- Addison's Disease
Increased CAR is associated with the following conditions:
- Visceral obesity in men
- Major depressive episodes
- Upper respiratory illnesses
- Bipolar disorder
- Fibromyalgia in women reporting abuse during childhood
- Women with BPD (borderline personality disorder)
- Smoking (to a small degree)
- Light exposure during waking
- Chronic stress and worrying
- Work overload

CAR Use in Monitoring Therapy
CAR may even be applicable in monitoring the efficacy of drug therapies used to treat these diseases. A recent study on the effects of the SSRI paroxetine on salivary cortisol in major depressive disorder reported a "robust CAR increase especially when patients became remitters versus no change in non-remitters during paroxetine treatment" so CAR may additionally be used to assess clinical response to antidepressant therapy.
Given the results of this study, it makes sense that CAR could be a powerful marker to monitor during the treatment of a dysfunctional HPA axis.
Problems With The CAR
As with anything that potentially gives us more information, interpretation can be tricky. Most people (about 75%) have a normal CAR and the remaining 25% do not. Different types of stressors affect CAR in different ways – chronic stress as opposed to acute, perceived, or social stress, or work overload, for instance.
Additionally, many normal things can affect the CAR. For example, collecting saliva on a less stressful non-work day very likely will yield a lower CAR. Finally, and perhaps most importantly, those individuals who have great difficulty conjuring the 1 mL volume of saliva required for the test may run into problems appreciating the CAR, because a single waking sample collected over a 15 or 30-minute time frame would actually represent more of an average.
Comparing average waking cortisol within the first 5 minutes with a second measure at 30 minutes and a third at 60 min could result in underestimation of CAR and compromise the usefulness of this test.
Sample Collection for Determining CAR
Simple to collect, all in all, the CAR could be a very useful addition to a salivary diurnal cortisol test.
From a laboratory perspective, the sampling required to determine the CAR is rather simple. It requires a saliva collection of about 1 mL without bubbles upon morning waking within the first 5 minutes, the second sample also of 1 mL without bubbles at 30 minutes, and a third sample at 60 minutes. Samples should be collected as quickly as possible (within a 5-minute time frame). The rest of the diurnal rhythm can be assessed at the normal time intervals (noon, evening, and night), making a total of 6 collection tubes.
Alternatively, when using a 4-tube collection, collect samples on waking, waking + 30 min, noon or evening, and night. For assessing CAR most accurately remember we're looking for the delta from morning waking to + 30 min and then + 60 min.
When monitoring the CAR in patients with conditions correlated with prolonged CARs, it may make sense to observe free cortisol at an additional time point 60 minutes after waking.
The Lab Me report always provides cortisol levels both numerically and graphically with results plotted against time of collection. Simple to collect, all in all, the CAR could be a very useful addition to a salivary diurnal cortisol test. The only thing left is to order some extra vials!
Take The Next Step
Try the Sleep Scanner test from Lab Me to get a detailed view of your daily cortisol fluctuations. Lab Me premium tests such as the Sleep Scanner, Advanced Neurotransmitters, Heavy Metal Toxicity, and Comprehensive Thyroid all include medical support.
If you would like to measure just cortisol 4x throughout the day let us know by sending an email here and we will happily help you do so.
Meaning you are able to ask us any question about your report and our medical staff will answer for no extra charge.


